Why Serotonin-Based Antidepressants Don’t Work Right Away
- Feb 23
- 3 min read
Written By Boyoung Park

Many people start antidepressants hoping for quick relief, yet find that nothing feels different even after weeks. This article looks at why serotonin-based medications work more slowly than we expect, and what that delay tells us about how complex depression really is.
Why Serotonin-Based Antidepressants Don’t Work Right Away
Antidepressants are well known to “balance” brain chemicals signals. One of their main targets is serotonin, a neurotransmitter involved in mood regulation. If serotonin levels increase soon after taking antidepressants, it seems reasonable to expect immediate relief. Yet for most people, emotional improvement takes weeks. This delay raises a simple but important question: why does altering serotonin signaling at the synapse lead to gradual, rather than instant recovery?
Serotonin is a neurotransmitter that plays a major role in regulating mood, anxiety, and emotional stability. Under normal conditions, serotonin is released from the presynaptic neuron into the synaptic cleft, a site where neurotransmitters bind to receptors and transmits a signal.
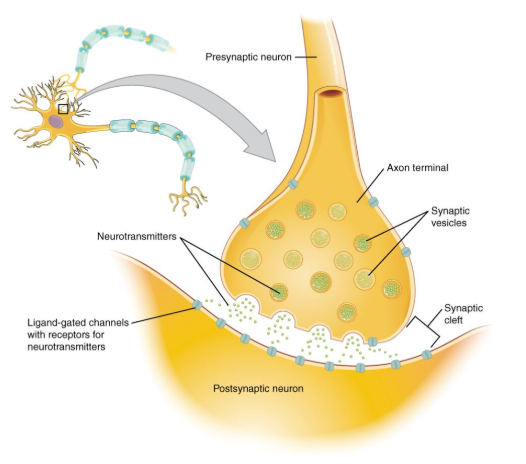
Figure 1. Diagram of a chemical synapse showing synaptic vesicles releasing neurotransmitters from the presynaptic neuron into the synaptic cleft, where they bind to specific receptors on the postsynaptic neuron.
Source: Anatomy Note.
After a signal is transmitted, serotonin is removed from the synaptic cleft by the process reuptake, which ends the signal. SSRIs tend to slow this reuptake, by allowing serotonin to remain active for longer and continue affecting the receiving cell. This extends the signal and slightly increases the overall effect of serotonin. Over time, these prolonged signals can contribute to gradual changes in brain activity involved in mood and emotional regulation.

Figure 2. Effect of SSRIs at the synapse.
Selective serotonin reuptake inhibitors (SSRIs) block the serotonin transporter, increasing synaptic serotonin availability and prolonging receptor stimulation
At first glance, this process seems simple: it seems that more serotonin in the synapse should lead to better mood-related signaling. However, clinical observations demonstrate that this explanation is not complete. Although serotonin reuptake is inhibited shortly after taking SSRIs, noticeable improvement in depressive symptoms usually takes several weeks. This delay suggests that increased serotonin levels alone cannot fully explain how these medications work.
A possible explanation involves gradual changes within the serotonergic system, which is the brain network that uses serotonin for signaling. When serotonin levels remain elevated for long periods of time, the serotonergic system adjusts how they respond. These changes can influence gene activity and promote the production of proteins that strengthen neuronal connections, particularly in brain regions involved in emotional regulation. This theory directly supports the delayed effects of serotonergic activity.
Despite their effectiveness, SSRIs also have clear limitations. Some patients do not respond to treatment, and others experience side effects like sleep problems or emotional blunting. This suggests that increasing serotonin signaling does not always improve emotional processing. In addition, depression encompasses a wide range of symptoms, and many cannot be adequately explained by serotonin imbalance alone. This challenges the idea that depression can be fully understood through the role of a single neurotransmitter.
Moreover, focusing solely on serotonin might limit how depression is understood. Emphasizing a single neurotransmitter risks overlooking other critical factors, such as stress, environmental influences, or individual differences in brain function. This narrow focus is likely to slow down personalized and effective approaches in mental health treatment.
Recognizing these limitations is critical in psychiatry, where treatment responses depend on individual differences in brain function. SSRIs not only indicate that altering serotonin reuptake can support recovery, but also highlight the difficulty of linking molecular changes in the brain to personal emotional experience.
References:
Moncrieff, J., Cooper, R. E., Stockmann, T., Amendola, S., Hengartner, M. P., & Horowitz, M. A. (2022).
The serotonin theory of depression: a systematic umbrella review.
Molecular Psychiatry, 27, 240–258.
National Institute of Mental Health. (n.d.). Mental health medications.
Neuroscientifically Challenged. (n.d.). The serotonin hypothesis and neurogenesis.
Harvard Health Publishing. (n.d.). What you should know about antidepressants.
.png)



Comments